As a cancer survivor, replacing any teeth you lost before, during, or after treatment can be an important part of regaining your health and quality of life. For many patients, dental implants are an excellent option – but the process requires some special considerations for cancer patients (i.e., is it possible for chemotherapy and dental implants to happen during the same time period?).
This is especially true for those who are currently battling breast cancer or who have battled breast cancer, the most commonly diagnosed cancer among American women. In my 25 years of dental implant surgery experience, here is what cancer patients need to know about getting dental implants.

Breast cancer survivors may face additional challenges when it comes to dental implants, especially if they received radiation therapy to the head, neck, or chest area. Other common cancers like lung, prostate, and colorectal cancers can also impact dental implant treatment depending on the location of radiation and types of treatments received. No matter the cancer type, careful planning is essential for a successful outcome.
The Challenges of Cancer Therapies as it Relates to Chemotherapy and Dental Implants
Both chemotherapy and radiation therapy can impact the body’s ability to heal properly from the dental implant or bone graft surgery. This increases the risk of complications like implant failure or infection.
Chemotherapy works by targeting rapidly dividing cells – including healthy cells involved in wound healing and bone regeneration. This can delay healing and interfere with the implant’s ability to integrate with the jawbone and cause implant failure.
Typically, dental implant surgery is not done during the chemo period, but the restorative teeth-making part can be completed if timed at the end of each chemotherapy cycle.
Radiation to the Head/Neck/Chest
Radiation therapy to the head, neck, or chest area can damage bone cells and blood vessels in the jaw. This reduces the quantity and quality of the bone available for implant placement. Radiation can also reduce blood flow, which is critical for healing. Breast cancer patients typically do not get radiation to the upper or lower jaw, so it is usually not a problem for this type of cancer.
However, these challenges don’t necessarily rule out dental implants entirely. With proper planning and timing, most cancer survivors can be excellent candidates!
For those who received radiation to the jaw area, we may use hyperbaric oxygen therapy prior to implant surgery to promote better healing and bone integration.
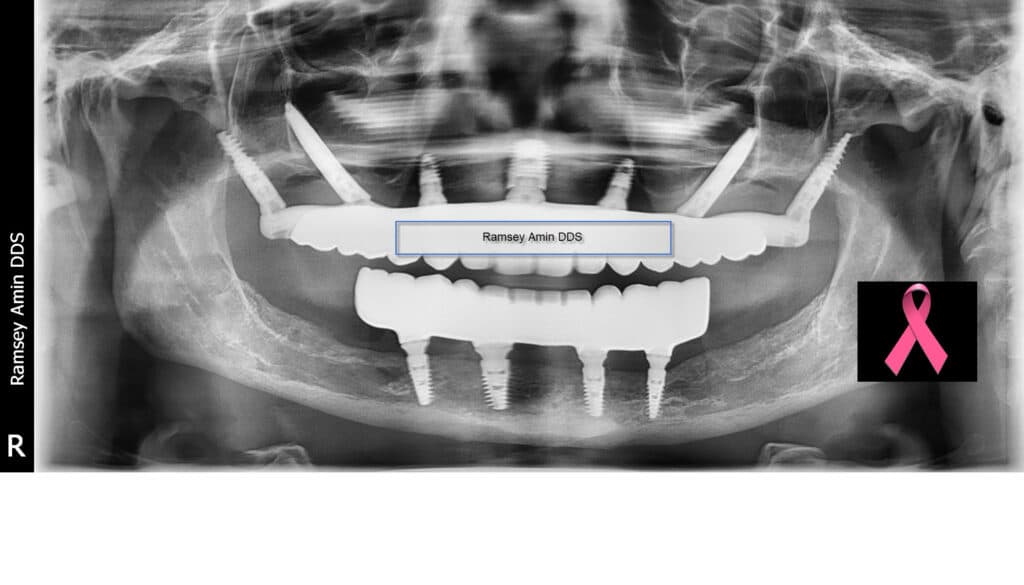
Cancer patient with full arch dental implants – Ramsey Amin DDS
Immunotherapy vs Chemotherapy
For breast cancer patients treated with immunotherapy drugs like Herceptin (trastuzumab) for HER2+ cancer, there are some additional considerations:
Herceptin (Trastuzumab)
Herceptin is a targeted therapy that binds to the HER2 receptor on cancer cells to prevent them from growing. Unlike chemotherapy, it does not directly impact rapidly dividing cells involved in wound healing. However, it can still slightly increase dental infection risk by altering the immune response.
Patients on Herceptin may be at a slightly lower risk for implant healing complications compared to chemotherapy. However, careful monitoring is still needed, as Herceptin can potentially be given with chemotherapy drugs as part of a treatment regimen.
The timing of implants in relation to Herceptin cycles is important. Your oncologist and dental implant specialist will coordinate to find the ideal window for implant surgery. It is not uncommon for chemo to end and Herceptin immunotherapy to continue.
Timing With Breast Reconstruction
For breast cancer survivors, it’s important also to consider the timing of any breast reconstruction procedures. Ideally, dental implants should be completed before or after breast reconstruction to avoid any surgical complications or interference between treatment areas.
Your cancer team will help coordinate the ideal sequencing. Oftentimes, the procedure can be partially completed during the tissue expander phase if a mastectomy is needed.
Waiting Period After Treatment
To give your body adequate time to recover, most experts recommend waiting a few months after completing chemotherapy or radiation before getting dental implants. This allows your healing ability and immune function to return closer to normal levels.
Keep in mind that some dental implant procedures are easy, like a single tooth molar, versus something more complex, like a sinus lift bone graft or full mouth implant replacement.
Higher Risk Situations
Certain cancer types, treatments, and medications can make dental implants more risky, at least initially after treatment. For example:
- Bone marrow/stem cell transplants can lead to prolonged healing issues
- Immunosuppressant medications may need to be adjusted or discontinued temporarily
- Head/neck/chest radiation
- IV Bisphosphonate drugs used for metastatic bone disease can interfere with implant healing
In these higher-risk cases, we may need to delay implants until healing ability has recovered sufficiently or possibly consider not having dental implants and just having traditional dentures or bridges.
The Importance of a Team Approach
Placing dental implants in a cancer survivor or a current cancer patient requires a collaborative, team-based approach involving your oncologist, plastic surgeon, and dental implant specialist.
This multi-disciplinary team will work together to develop a treatment plan that maximizes your chances for successful implant integration while minimizing risks. We’ll also take into account any future cancer treatments you may need to ensure they don’t compromise your dental implants.
Proper Timing is Critical
One of the most important factors for success is timing your implant procedure correctly in relation to your cancer treatment schedule. Getting dental implants DURING chemotherapy or radiation can significantly increase failure rates and is never a good idea.
Waiting until your healing ability has recovered is crucial. Depending on your situation, this may mean delaying implants for several months or longer. Your oncologist and dental implant specialist will closely monitor you and consult for implant surgery when the time is right.
Hormone replacement therapy (HRT) after breast cancer can have an impact on dental health and procedures like implants and bone grafting. Estrogen deficiency, which HRT addresses, can lead to bone loss and affect the jawbone’s health, potentially complicating dental implants and bone grafting. However, HRT may help improve bone density, which can be beneficial for the success of these dental procedures.
Dental Implants Can Restore Smiles After Cancer
With the proper precautions, timing, and experienced treatment team, many cancer patients and survivors can be excellent candidates for dental implants – including those who have battled breast cancer, lung cancer, prostate cancer, colorectal cancer, and other common cancer types.
Dental implants can help restore function, confidence, and quality of life after battling cancer.
The key is working with a dental implant specialist who has in-depth experience treating patients with complex medical histories like yours.
If you’re a cancer survivor interested in dental implants, visit our Find-A-Dentist tool to locate an AAID-credentialed dental implant expert near you. Everyone reading this has had a friend or a family member impacted by cancer. I pray that during my career, a cure is found.
Take the quiz to learn why you can count on an AAID-credentialed dentist.
 Dr. Ramsey Amin, DDS, FAAID, DABOI/ID, maintains an implant-only practice in Burbank, California. He performs all "full-scope implantology" with prosthetic reconstructions, including zygomatic and pterygoid implants. He is the President of the AAID Western District and can be reached at https://www.burbankdentalimplants.com.
Dr. Ramsey Amin, DDS, FAAID, DABOI/ID, maintains an implant-only practice in Burbank, California. He performs all "full-scope implantology" with prosthetic reconstructions, including zygomatic and pterygoid implants. He is the President of the AAID Western District and can be reached at https://www.burbankdentalimplants.com.